Why Healthcare AI Fails to Deliver ROI (And How to Fix It)
Healthcare organizations are investing billions into AI in healthcare, yet many leaders quietly admit the same frustration: “Where is the ROI?”
Despite deploying predictive models, automation tools, and advanced analytics, outcomes often fall short cost savings are unclear, workflows remain inefficient, and clinicians resist adoption. At the same time, the pressure to AI development is increasing as healthcare systems demand faster deployment, lower costs, and measurable value from every digital initiative.
The reality is that many organizations approach AI as a technology upgrade rather than a strategic transformation. They invest heavily in tools but overlook critical factors such as workflow integration, data readiness, and change management. As a result, even technically sound AI solutions fail to deliver meaningful business outcomes.
This article breaks down why Healthcare AI ROI often fails and more importantly, how to fix it with modern, proven strategies.
Key Challenges Blocking Healthcare AI ROI
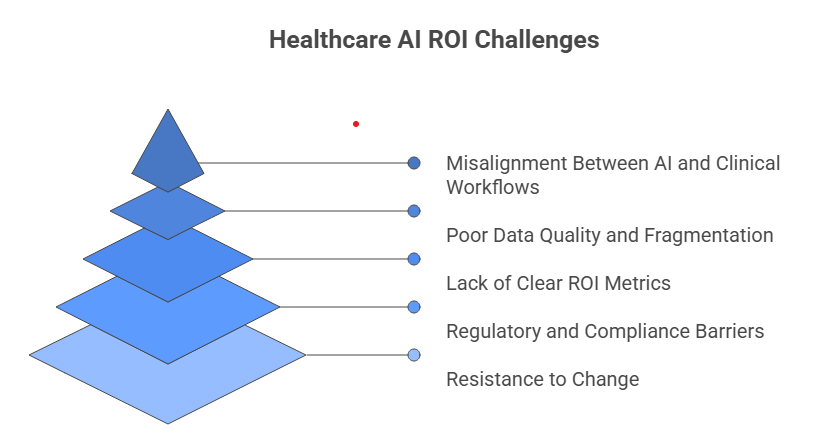
Misalignment Between AI and Clinical Workflows
Many AI solutions are designed without a deep understanding of how clinicians actually work. Hospitals operate in high-pressure environments where efficiency and accuracy are critical. If AI tools disrupt rather than support these workflows, adoption suffers.
Impact:
- Clinicians ignore or bypass AI recommendations
- Increased cognitive load instead of efficiency gains
- Workflow disruptions leading to frustration and resistance
Poor Data Quality and Fragmentation
Healthcare data is often spread across multiple systems EHRs, lab systems, imaging platforms creating silos that limit AI effectiveness. Inconsistent formats and incomplete datasets further degrade model performance.
Impact:
- Inaccurate predictions and unreliable insights
- Reduced trust in AI systems
- Increased time spent on data preprocessing rather than value creation
Lack of Clear ROI Metrics
Major reason AI initiatives fail is the absence of clearly defined success metrics. Organizations often deploy AI without aligning it to financial or operational goals.
Impact:
- Difficulty in measuring success
- Leadership skepticism toward AI investments
- Inability to justify scaling initiatives
Regulatory and Compliance Barriers
Healthcare is one of the most regulated industries. Compliance requirements around data privacy, security, and governance can delay or complicate AI deployment.
Impact:
- Slower innovation cycles
- Increased implementation costs
- Limited experimentation with new AI models
Resistance to Change
AI adoption requires cultural transformation. Clinicians and staff may view AI as a threat to their roles or an additional burden rather than a support system.
Impact:
- Low adoption rates
- Underutilization of deployed solutions
- Failure to achieve expected ROI
Emerging Tech Trends Solving the Problem
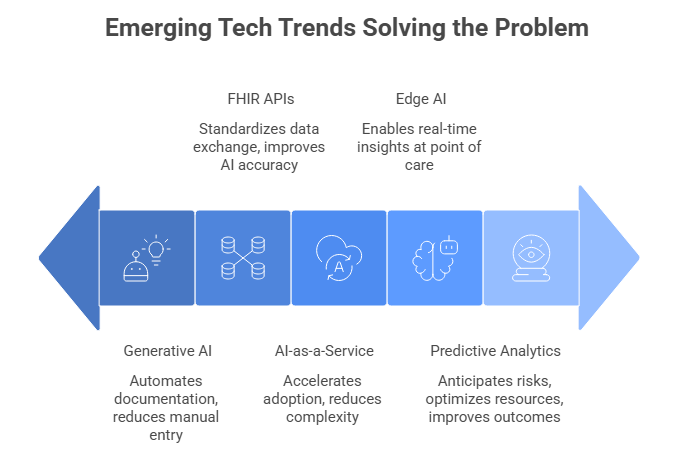
AI-Powered Predictive Analytics
Modern predictive analytics in healthcare is evolving into a critical tool for proactive decision-making. Hospitals are using it to anticipate patient risks, optimize resources, and improve care outcomes.
- Early detection of chronic diseases
- Prediction of patient deterioration
- Optimization of hospital resource allocation
Generative AI for Clinical Documentation
Generative AI is transforming administrative workflows by automating clinical documentation. This significantly reduces the time clinicians spend on manual data entry.
Interoperability with FHIR APIs
FHIR-based architectures are addressing one of the biggest barriers in healthcare data fragmentation. By enabling standardized data exchange, these systems improve AI model accuracy and usability.
Edge AI & Real-Time Decision Systems
AI is increasingly being deployed at the point of care, enabling real-time insights in critical environments such as ICUs and emergency response systems.
AI-as-a-Service Platforms
Organizations can accelerate AI adoption by leveraging scalable, compliant solutions developed by App Maisters, enabling faster deployment, reduced development complexity, and seamless integration with existing healthcare systems while maintaining long-term flexibility.
Step-by-Step Solutions to Achieve Healthcare AI ROI
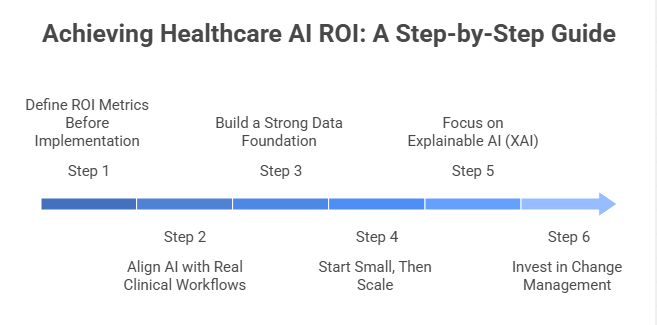
Step 1: Define ROI Metrics Before Implementation
Establish clear, measurable KPIs aligned with business outcomes:
- Reduction in patient readmission rates
- Improvement in diagnostic accuracy
- Decrease in operational costs
- Time saved per clinician
Tie these metrics directly to financial performance to ensure accountability.
Step 2: Align AI with Real Clinical Workflows
Design AI systems that integrate seamlessly into existing processes:
- Embed AI into EHR systems
- Provide decision support at the point of care
- Minimize disruption to clinician routines
Step 3: Build a Strong Data Foundation
Invest in data infrastructure that supports AI scalability:
- Standardize data using FHIR and HL7 protocols
- Implement robust data governance frameworks
- Ensure data accuracy, completeness, and consistency
Step 4: Start Small, Then Scale
Adopt a phased implementation approach:
- Launch pilot projects in targeted departments
- Measure performance against defined KPIs
- Refine models and workflows
- Scale based on proven success
Step 5: Focus on Explainable AI (XAI)
Transparency is critical for clinician trust:
- Use interpretable models
- Provide clear explanations for AI-driven decisions
- Enable clinicians to validate AI outputs
Step 6: Invest in Change Management
Successful AI adoption strategies require cultural alignment:
- Provide training and education programs
- Communicate benefits clearly
- Involve clinicians in the development process
Real-World Use Cases
- Predictive Patient Readmission: Hospitals are using AI models to identify high-risk patients before discharge. By enabling early interventions, these systems significantly reduce readmission rates and associated costs.
- AI in Radiology: AI-powered imaging tools assist radiologists in analyzing scans more efficiently. These systems enhance accuracy and reduce diagnostic delays, improving patient outcomes.
- Operational Efficiency with AI: AI-driven scheduling and resource management systems optimize staffing, reduce patient wait times, and improve overall operational efficiency.
- Virtual Health Assistants: AI-powered assistants handle patient queries, appointment scheduling, and follow-ups, reducing administrative workload and improving patient engagement.
Best Practices & Expert Tips
- Focus on Value, Not Hype: Prioritize AI initiatives that address real business problems and deliver measurable outcomes.
- Collaborate Across Teams: Effective implementation requires coordination between IT teams, clinicians, and business leaders to ensure alignment and success.
- Continuously Monitor AI Performance: AI systems require ongoing evaluation to stay accurate and effective, including tracking performance metrics, updating models with new data, and adapting to changing clinical needs.
- Ensure Compliance by Design: Integrate security and compliance measures from the beginning to avoid costly delays and risks.
Common Mistakes to Avoid
Overengineering AI Solutions
Complex models are not always better. Simpler, well-optimized solutions often deliver more reliable and scalable results in healthcare settings, especially when data quality is inconsistent. Overly complex systems also increase maintenance costs and make troubleshooting more difficult.
Ignoring User Experience
If AI tools are not intuitive and easy to use, adoption will remain low regardless of their capabilities. Poor interface design, lack of workflow integration, and excessive alerts can frustrate clinicians and lead to underutilization of the system.
Lack of Training and Education
Without proper training, even the most advanced AI systems will fail to deliver value. Healthcare staff need clear guidance on how to interpret AI outputs, integrate them into decision-making, and understand their limitations to build trust and confidence.
Scaling Too Fast
Rapid scaling without validated success can lead to operational inefficiencies and financial losses. Expanding AI initiatives without refining models, workflows, and infrastructure often results in inconsistent performance and increased risk across departments.
Wrapping Up
Healthcare AI is at a critical inflection point where success is no longer defined by technological capability alone, but by the ability to deliver measurable outcomes at scale. The gap between investment and ROI can only be closed when organizations move beyond experimentation and focus on optimizing AI development, aligning solutions with clinical workflows, and building strong, interoperable data foundations.
As the industry evolves, advancements in real-time decision intelligence, explainable AI, and connected data ecosystems will continue to accelerate adoption and value creation. At App Maisters, the focus is on enabling healthcare providers to turn AI into a practical, scalable asset bridging the gap between innovation and real-world impact. Ultimately, the organizations that succeed will be those that treat AI not as a standalone initiative, but as a strategic driver of efficiency, innovation, and patient-centric care.
FAQs
Why does AI in healthcare often fail to deliver ROI?
AI in healthcare often fails to deliver ROI due to poor data quality, lack of workflow integration, unclear KPIs, and low user adoption. App Maisters addresses these challenges by building scalable AI solutions aligned with real clinical workflows and measurable business outcomes.
How can healthcare organizations improve AI ROI effectively?
Healthcare organizations can improve AI ROI by defining clear success metrics, starting with pilot projects, ensuring data readiness, and focusing on user adoption. App Maisters helps optimize AI development with strategies that ensure faster deployment and long-term value.
What are the biggest AI implementation challenges in healthcare?
The biggest AI implementation challenges include data fragmentation, regulatory compliance, integration with legacy systems, and resistance from clinical staff. App Maisters provides end-to-end AI implementation strategies that overcome these barriers and accelerate adoption.
How is predictive analytics improving healthcare outcomes?
Predictive analytics in healthcare enables early disease detection, reduces patient readmissions, and improves resource allocation. App Maisters leverages advanced predictive models to deliver actionable insights that enhance both clinical and operational efficiency.
What are the best AI adoption strategies for healthcare providers?
Effective AI adoption strategies include aligning AI with clinical workflows, investing in data infrastructure, using explainable AI, and implementing strong change management practices. App Maisters supports healthcare providers with tailored AI solutions designed for seamless adoption and scalability.
How can AI reduce operational costs in healthcare?
AI reduces operational costs by automating administrative tasks, optimizing staff scheduling, and improving resource utilization. App Maisters develops AI-driven systems that streamline operations while maintaining compliance and performance.
What is the future of AI in healthcare beyond 2026?
The future of AI in healthcare includes real-time decision intelligence, personalized patient care, and fully interoperable data ecosystems. App Maisters is at the forefront of delivering innovative AI solutions that help healthcare organizations stay competitive and ROI-focused in the evolving digital landscape.




















